Accelerating Claims Accuracy and Efficiency with AI-Powered Decision Support
Workers’
Compensation
Settlement Platform
Discover how MindInventory built an AI platform that transforms
unstructured medical
guidelines into accurate workers’ compensation claim decisions.
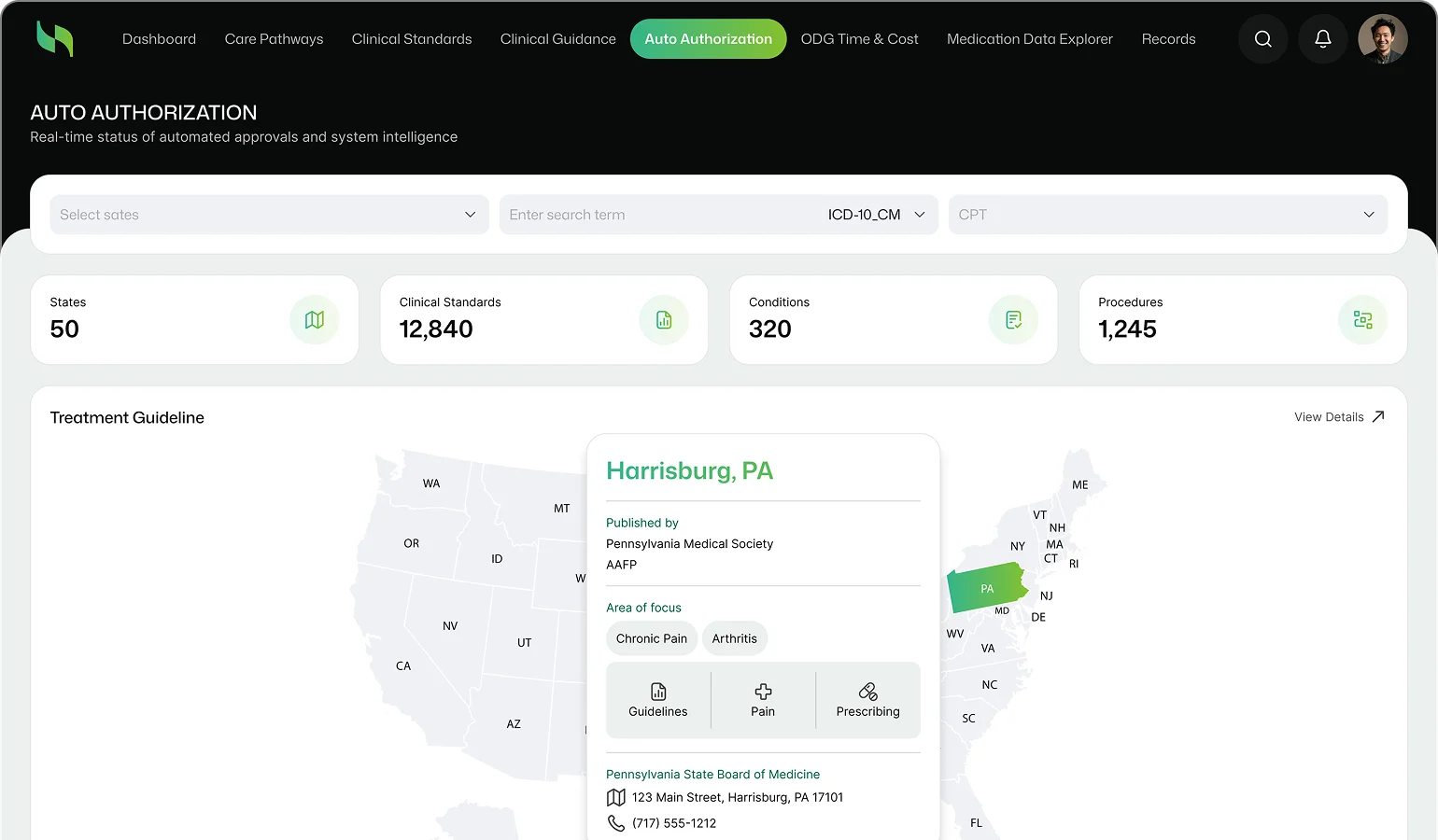
Project
Overview
A US-based medical claim processing management company set out to simplify and speed up workers’ compensation claim settlement across the United States. The challenge was not the lack of data but the lack of structure, consistency, and real-time usability across state-specific treatment guidelines published by multiple authorized bodies.
MindInventory partnered as the technology, data, and AI execution partner, translating the client’s product vision into a scalable, production-ready platform. The engagement focused on building a unified data and AI foundation that could convert unstructured medical and regulatory content into clear, actionable claim decisions for insurance providers operating nationwide.
Recruitment
pipeline that could:
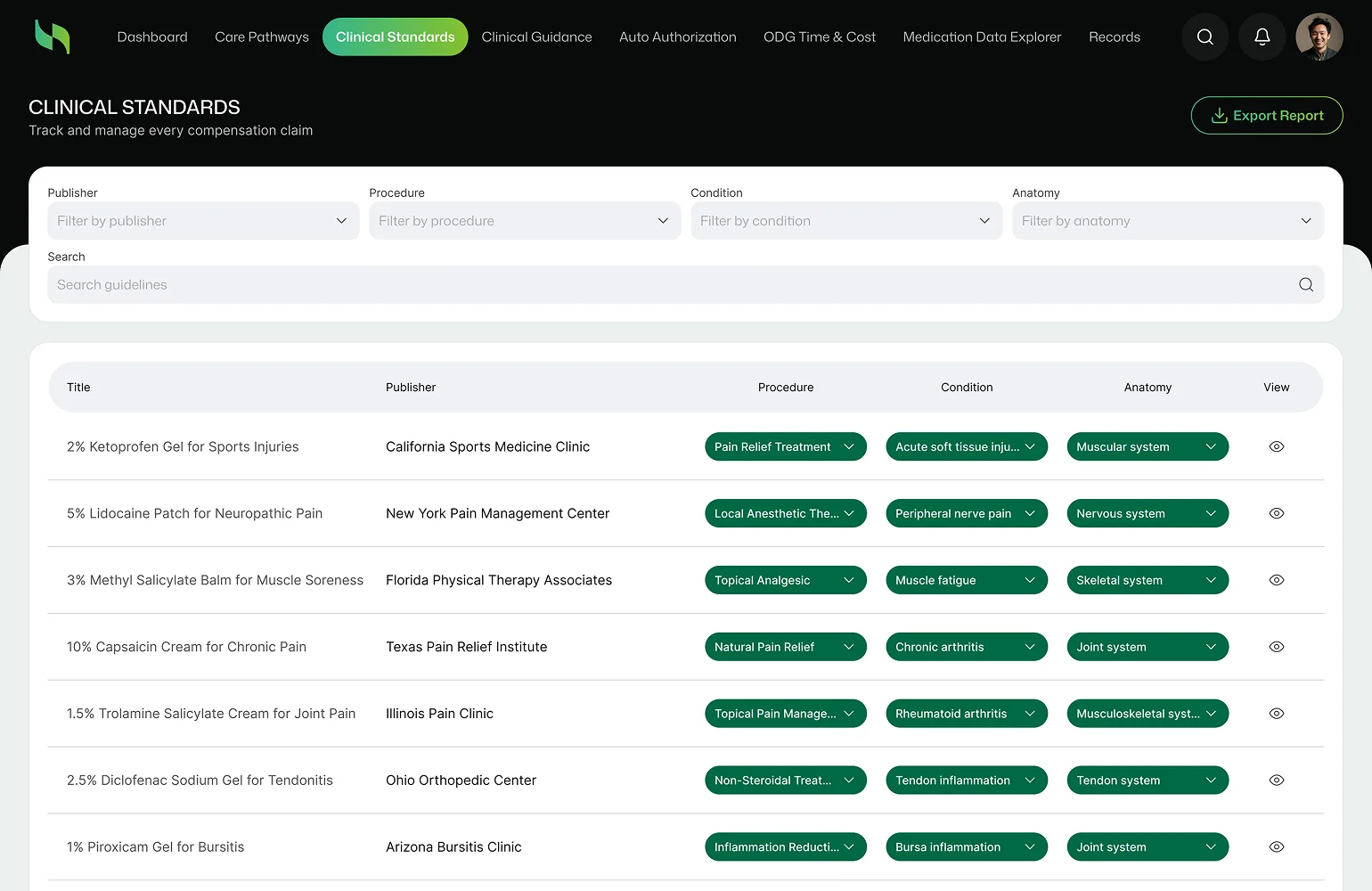
Challenges
data slowed claim processing efficiency.

Solution
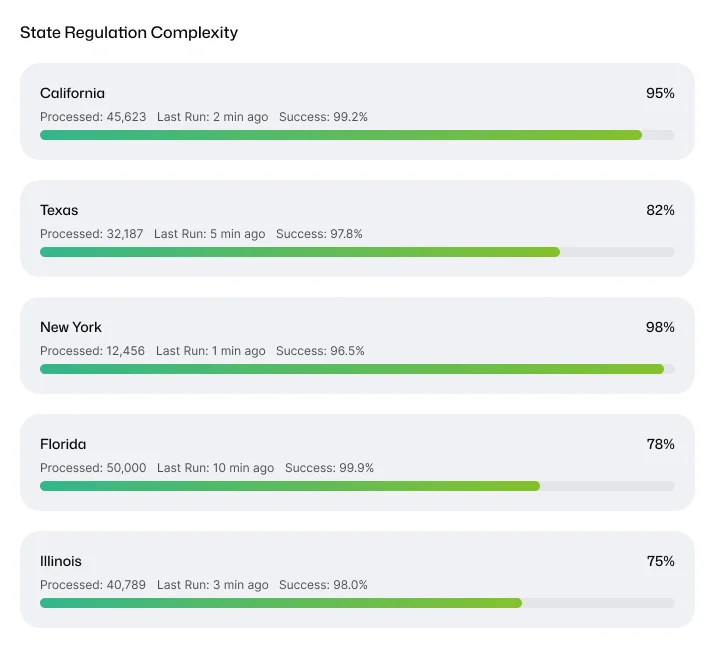


Strategic
Approach
Continuous Updates
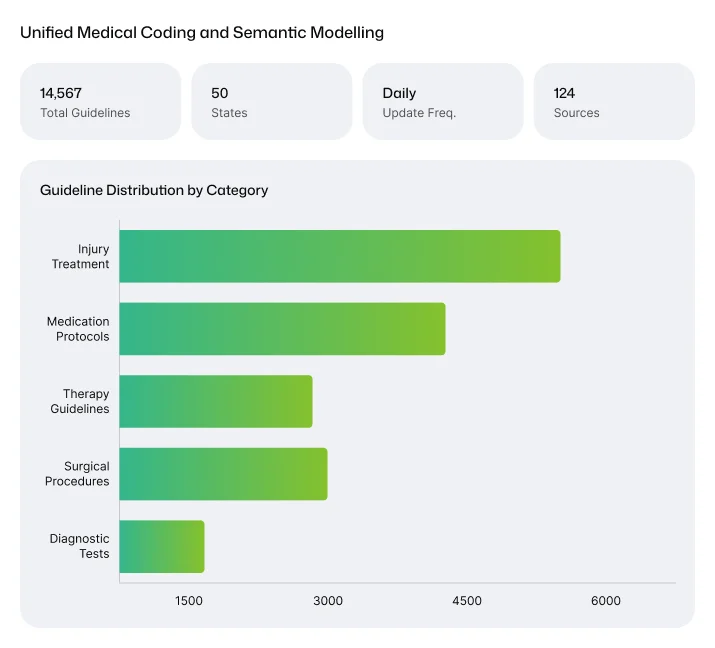
- Automated extraction of treatment guidelines from authorized publishers
- Regular updates to reflect changes in state regulations and evidence-based standards
- Centralized storage ensuring a single source of truth
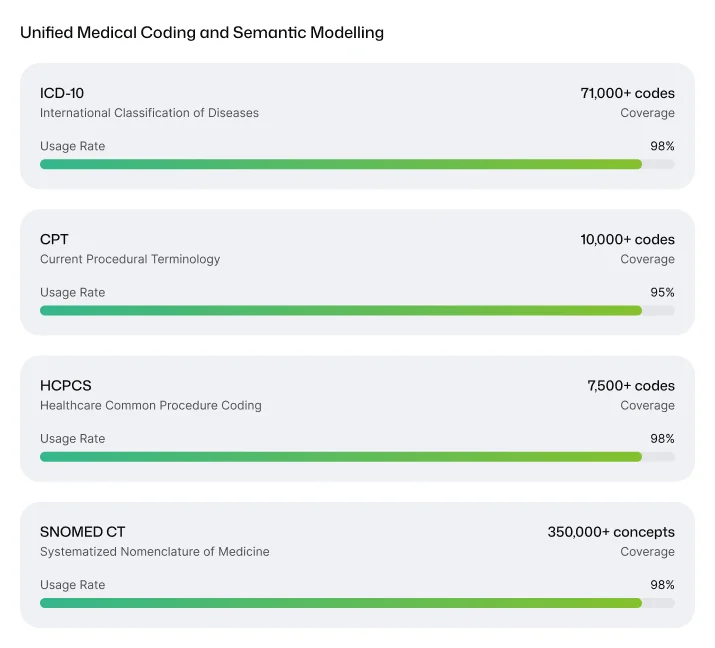
Structuring
- Hierarchical modeling of anatomy, conditions, and procedures
- Classification of procedures into therapeutic and surgical categories
- Mapping to ICD-10, CPT, HCPCS, RxNorm, and SNOMED relationships
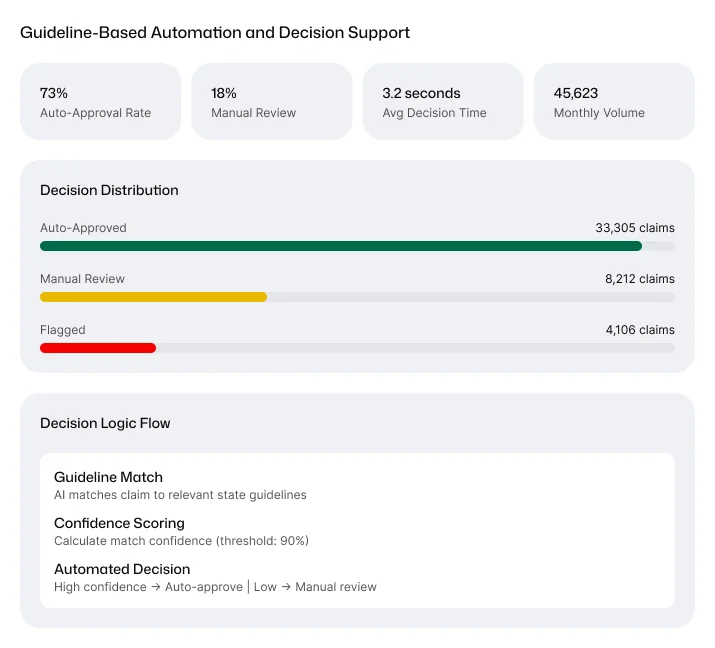
Engineering
- Prompt-driven interfaces for claim and utilization review teams
- Natural language input translated into structured, guideline-aligned outputs
- Reduced dependency on manual coding and clinical expertise
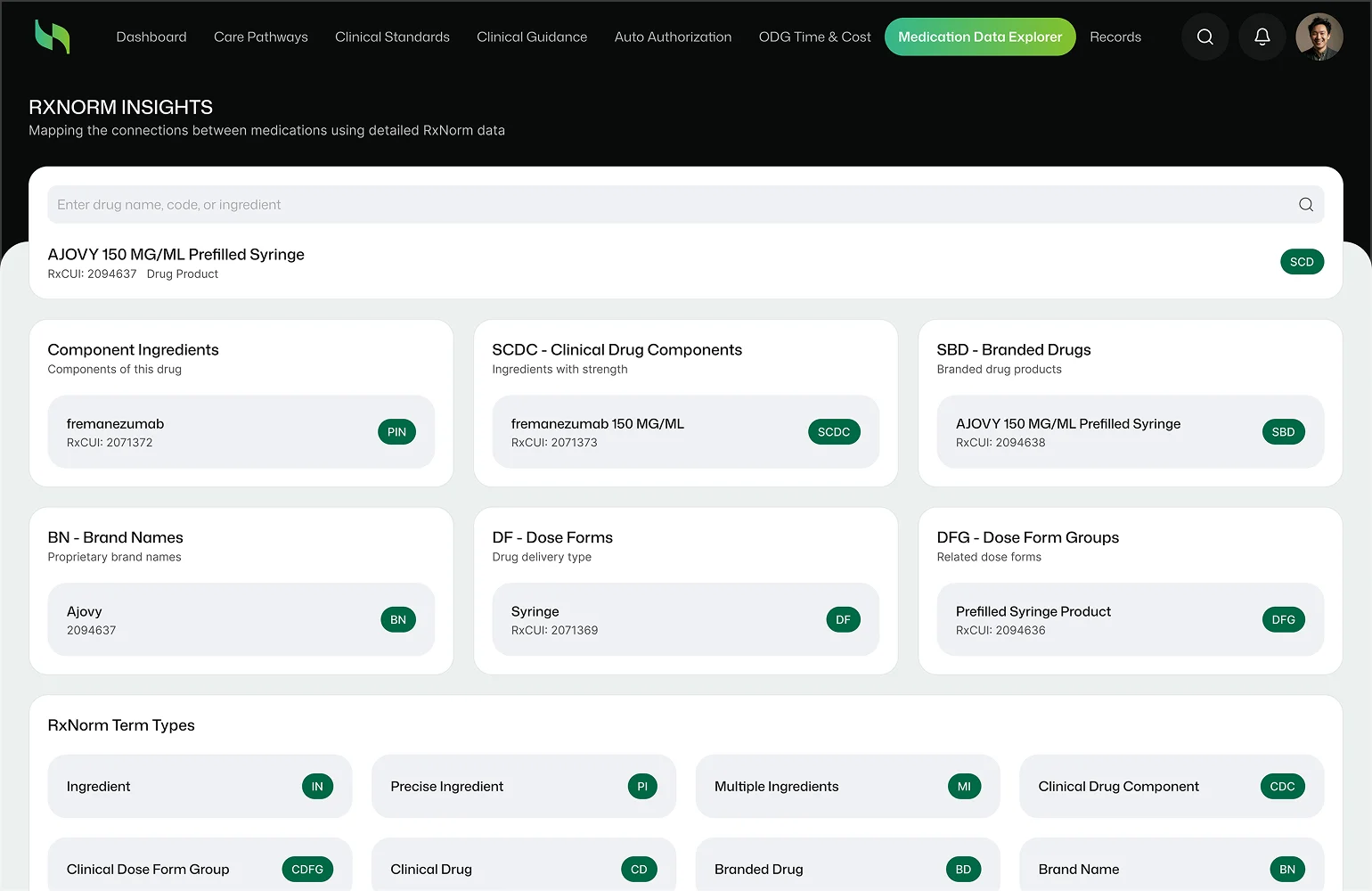
Impact
processing duration
handling
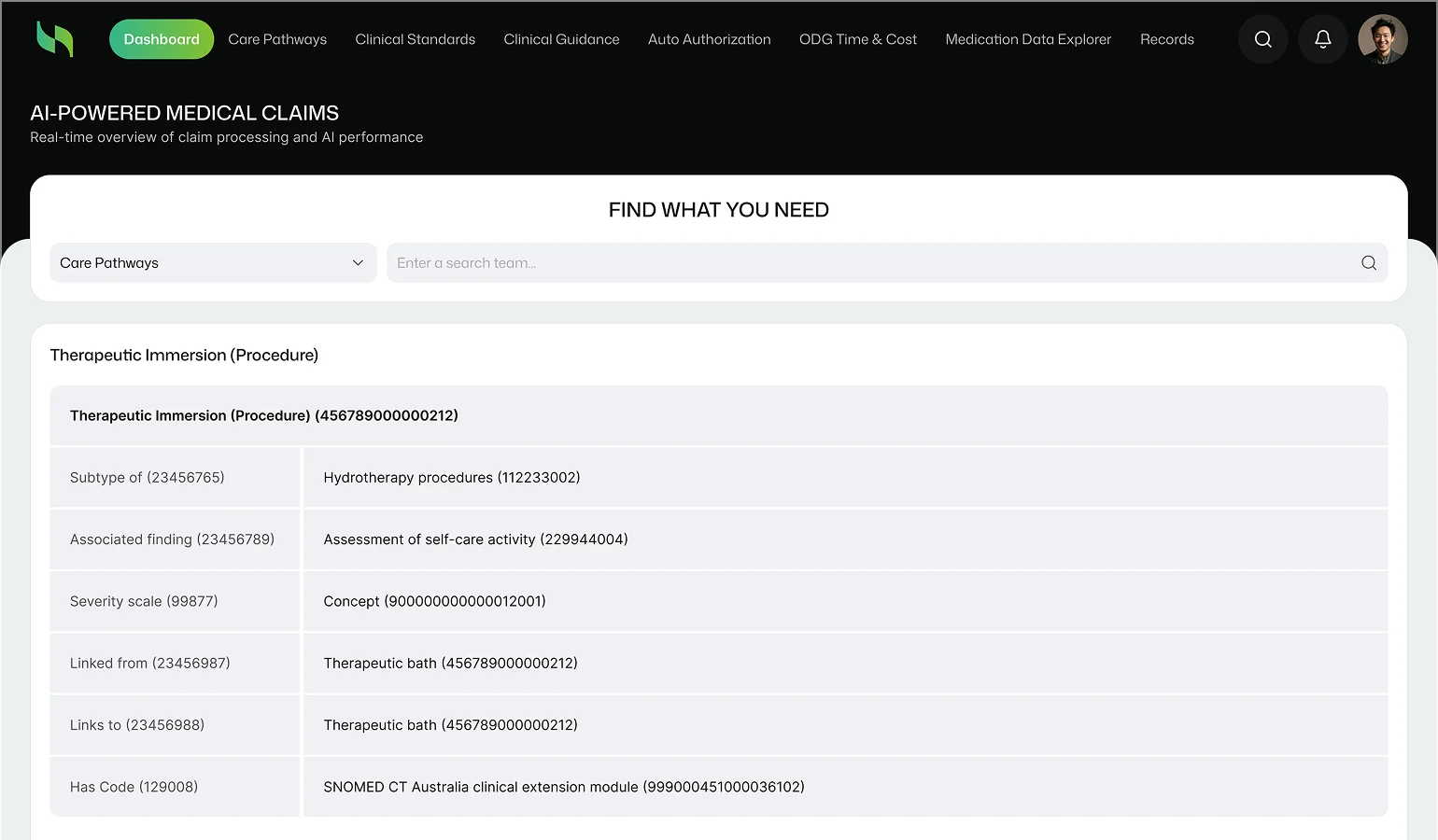
Managing Complex, Regulation-Heavy Processes Across Geographies?

